Multiple Sclerosis (MS) is a potentially devastating disease in which a person’s immune system attacks its own central nervous system resulting in inflammation of nerves, and potential permanent destruction of nerves.
The central nervous system is comprised of the spine and brain. The eyes are an extension of the brain, and therefore are considered a part of the central nervous system. This means that multiple sclerosis can, and frequently does, affect the eyes.
In fact, in up to 20% of cases, optic neuritis, or inflammation of the optic nerve, is the initial finding of multiple sclerosis—that’s in 1 out of 5 diagnoses!
Anatomy of the Eye
To understand MS and how it affects the eye, it is beneficial to have a basic understanding of how the eye works.
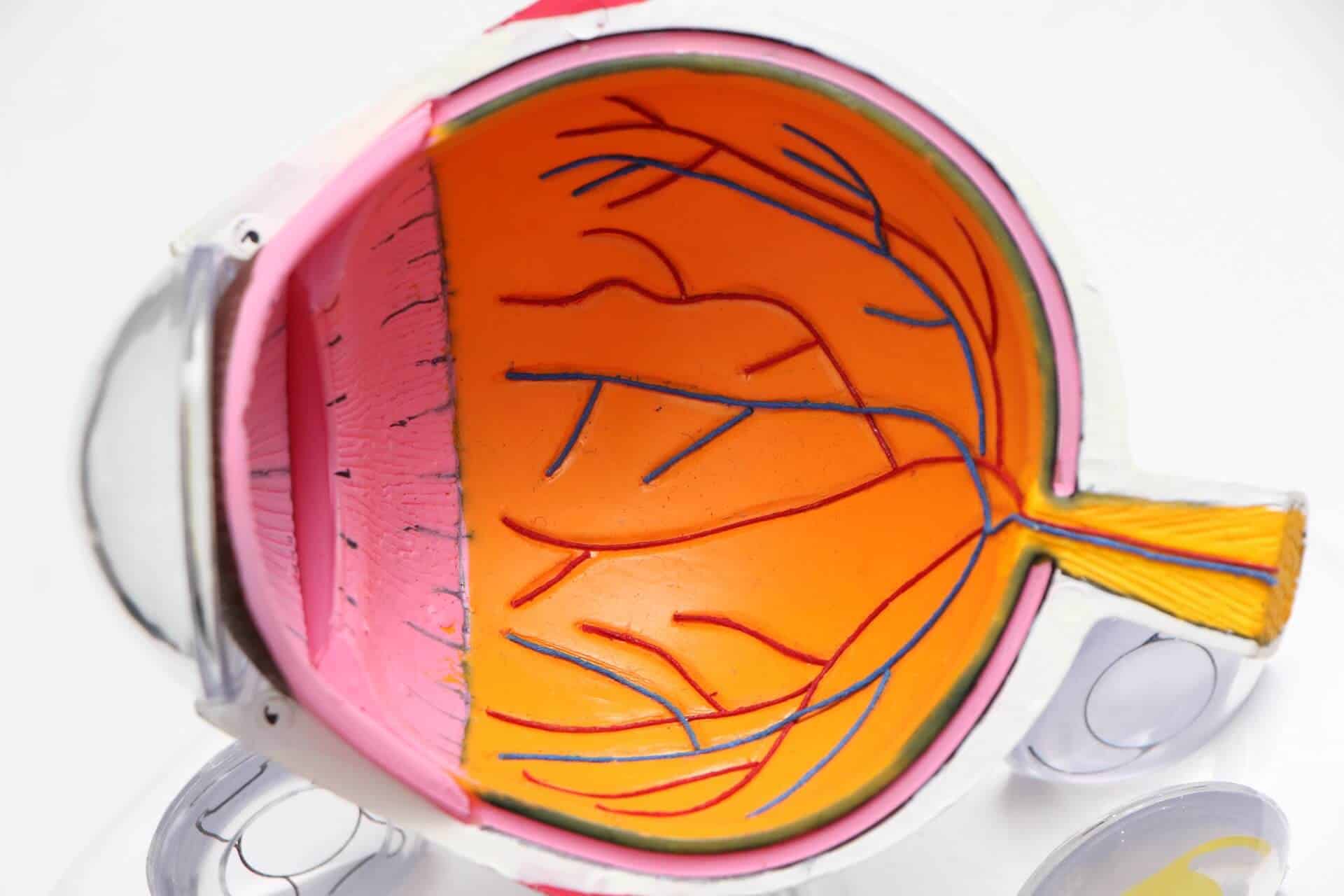
The eye creates vision based off of light landing as a point source on specialized cells called photoreceptors, which are located in the backmost structure of the eye—the retina.
The more photoreceptors stimulated by the light, the brighter, more colorful, and more well defined the image.
Photoreceptors send their signals to the brain via electrostimulation along axons.
Millions of axons combine together (similar to fibers making up a fiber optic cable) and exit the eye as a combined conglomerate “mega nerve” called the optic nerve.
The optic nerve then travels to the brain where the signals from the photoreceptors are processed to create visual images.
Multiple Sclerosis is a disease in which the body’s immune system attacks and destroys a structure called myelin.
Myelin is a coating that covers many nerves in the central nervous system and is responsible for increased transmission speed of signals to and from the brain.
The optic nerve is encompassed in myelin, which is how the eye can be involved in Multiple Sclerosis.
If the body attacks the myelin coating of the optic nerve, it can induce a problem called optic neuritis.
What is Optic Neuritis?
Optic neuritis is another way to say inflammation of the optic nerve.
It is not solely found in Multiple Sclerosis patients, it can occur on its own (idiopathic), or is sometimes seen in individuals with Lupus, Syphilis, Sarcoidosis, Behcet’s disease, Lyme disease, Herpes, Cat-Scratch Fever, and more.
Patients with optic neuritis may present with decreased vision, decreased brightness and/or color vision in the affected eye, and/or pain on eye movement.
These findings are common with optic neuritis because the optic nerve is swollen and inflamed. These conditions limit the number and strength of signals that can be transmitted from the eyes to the brain.
Therefore, optic neuritis becomes a conduction problem–the eye itself is functioning properly, and the brain is processing the information properly; however, the information is being “bottlenecked” resulting in decreased signals reaching the brain, hence causing decreased vision, decreased color strength and decreased brightness.
Pain is often noted on eye movement due to the inflammation of the nerve itself. Just like an inflamed muscle, any movement or strain put on an inflamed nerve can result in pain and irritation.
An additional finding that is seen with optic neuritis is an afferent pupillary defect (APD).
An APD is a finding in which the eyes do not correctly respond to light, as light is not being correctly transmitted to the brain in the affected eye.
For this reason, when light is shown into the affected eye, the pupil (black part of the eye) will not constrict as it normally would. Instead, the pupil remains large (dilates) in response to a light stimulus.
APD’s can be detected easily by a well-trained optometrist or ophthalmologist using a technique called “the swinging flashlight test”.
Essentially, the lights in the exam room are turned off. A small light source such as a penlight is shown into one eye for 3 seconds, the light source is then rapidly moved over to the other eye for 3 seconds. This process is repeated several times.
If an APD is present, the doctor will see a dilation of the affected pupil and constriction of the pupil in the unaffected eye.
The onset of optic neuritis can vary–it can be rapid (a patient wakes up with decreased vision) or it can slowly progress over the time span of a week.
To heal, optic neuritis can take anywhere from 1-3 months to completely resolve. Fortunately, in most cases vision returns back to normal baseline without long-term complications.
While uncommon, cases of optic neuritis can recur over time. Recurring episodes of optic neuritis is especially characteristic of Multiple Sclerosis.
Diagnosing Optic Neuritis
When it comes to optic neuritis, it can be a bit complicated to diagnose. To start, your eye doctor will want to perform a dilated fundus exam to carefully inspect the retina and opening of the optic nerve.
The optic nerve is 40 millimeters in length (from the eye to the brain). Of this 40 millimeters, only 1 millimeter is “intraocular”. In other words, 1 millimeter is located “within the eyeball” where an eye doctor could potentially see the inflammation, whereas the other 39 millimeters are located behind the orbit.
This means that the inflammation of the nerve cannot always be seen with dilation.
Optic neuritis is therefore separated into two subcategories–optic neuritis or retrobulbar optic neuritis. Optic neuritis refers to inflammation of the 1 millimeter intraocular section of the optic nerve. Retrobulbar optic neuritis refers to inflammation anywhere along the 39 millimeter section of optic nerve behind where an optometrist or ophthalmologist can see.
Cases of retrobulbar optic neuritis, therefore, are what are difficult to diagnose as the nerve (that the doctor can see) looks “normal”. Your doctor will need to rely on patient reported symptoms to point towards the correct testing for a retrobulbar optic neuritis diagnosis.
Testing for optic neuritis include MRI imaging, a visual field test, and careful examination of the eyes and optic nerves.
MRI imaging is also necessary for diagnosing Multiple Sclerosis. During an episode of optic neuritis, the risk of developing Multiple Sclerosis significantly increases with presence of white matter lesions on MRI scans.
In fact, studies have shown that there is a 50% chance of developing Multiple Sclerosis within 15 years following a diagnosis of optic neuritis.
This risk increases to 75% if one or more white matter lesions are found on MRI during an episode of optic neuritis.
On the other hand, this risk decreases to 25% if no white matter lesions are found on MRI during an episode of optic neuritis.
Therefore—MRI’s are very important tests that should strongly be considered in cases of suspected optic neuritis! MRI’s are not needed to diagnosis optic neuritis, but instead used to diagnose or predict the risk of developing Multiple Sclerosis.
How is Optic Neuritis Treated?
Optic neuritis will naturally resolve over the course of several months, therefore no treatment is technically “necessary”.
However, corticosteroids given via IV have been shown to increase the healing time of optic neuritis, returning vision closer to normal as quickly as within 2 weeks of the initiation of treatment.
This is not to be confused with steroid treatments given orally (via pills), as oral steroid treatment has actually been shown to increase the risk of recurrence of optic neuritis.
Ultimately, treatment will need to be decided based on concurrent other symptoms and be a discussion with you and your doctor.
Other Signs of Multiple Sclerosis
While optic neuritis is not diagnostic of Multiple Sclerosis, the two conditions are often interlinked.
Other unique signs associated with Multiple Sclerosis include Uthoff’s sign, Lhermitte’s sign, and the “MS Hug”.
Uthoff’s sign is a finding in which neurological deficits are noted with an increase in body temperature (seen with prolonged periods of exercise, when taking a hot shower or bath, in warm climates, etc.).
Examples of neurological deficits include worsening vision, balance problems, weakness or tingling of the extremities, cognitive changes, or even bladder problems.
Lhermitte’s sign is a finding in which an individual feels an “electric shock” sensation when the neck is bent forward. This shocking sensation can remain around the neck region, or may travel down the spine.
The MS Hug is the feeling of a tight band constricting the chest/rib region. This crushing feeling can present as a tickling or dull sensation or may progress to be a sharp or burning pain.
The MS hug can last for just a few seconds or hours at a time. It may affect just one side of the chest or encompass the entire midsection from the neck to the waist.
If you or someone you know thinks they may be suffering from optic neuritis or Multiple Sclerosis be sure to make an appointment with your doctor as soon as possible.